Detect Fraud, Waste, and Abuse Schemes
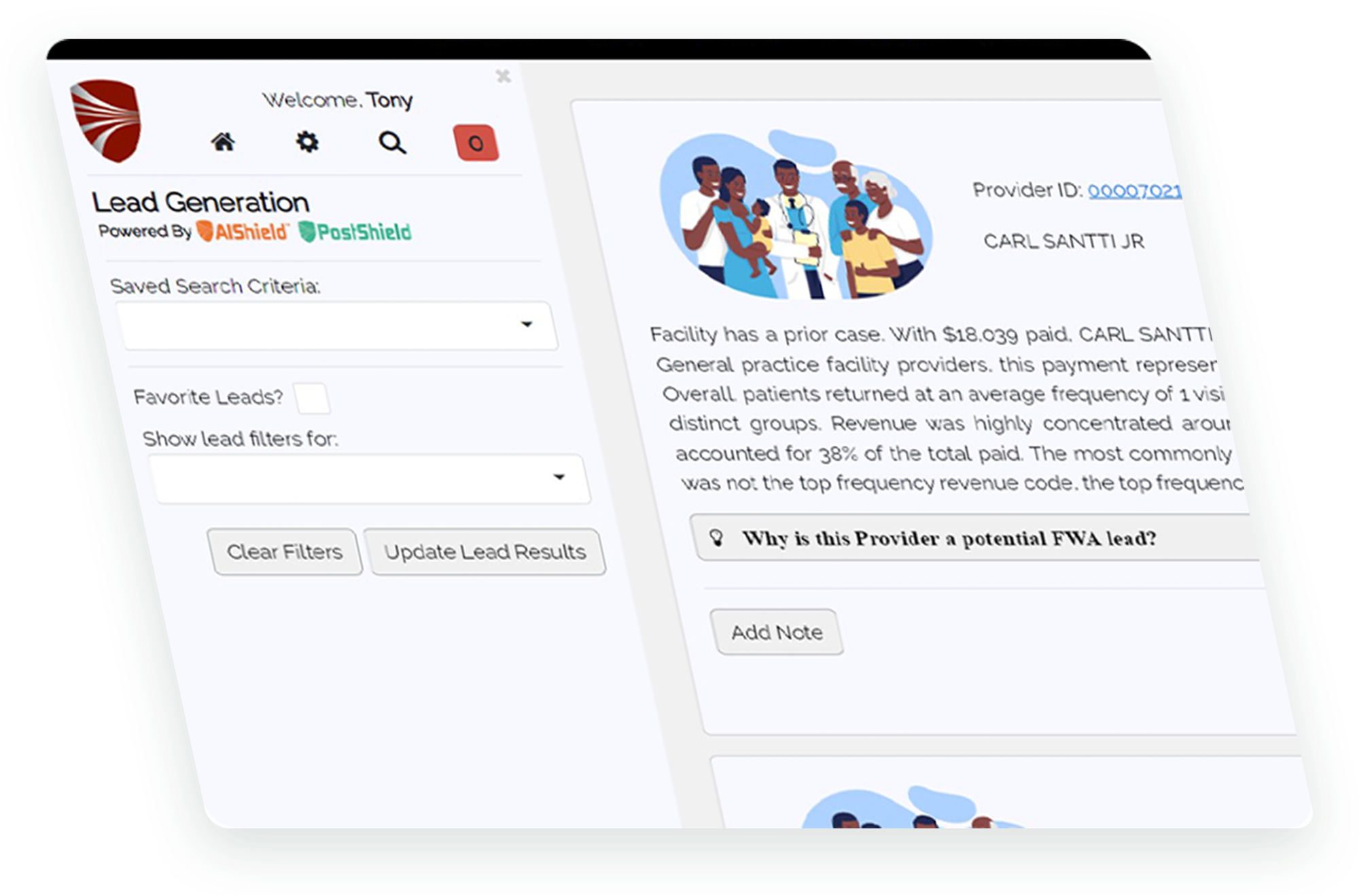
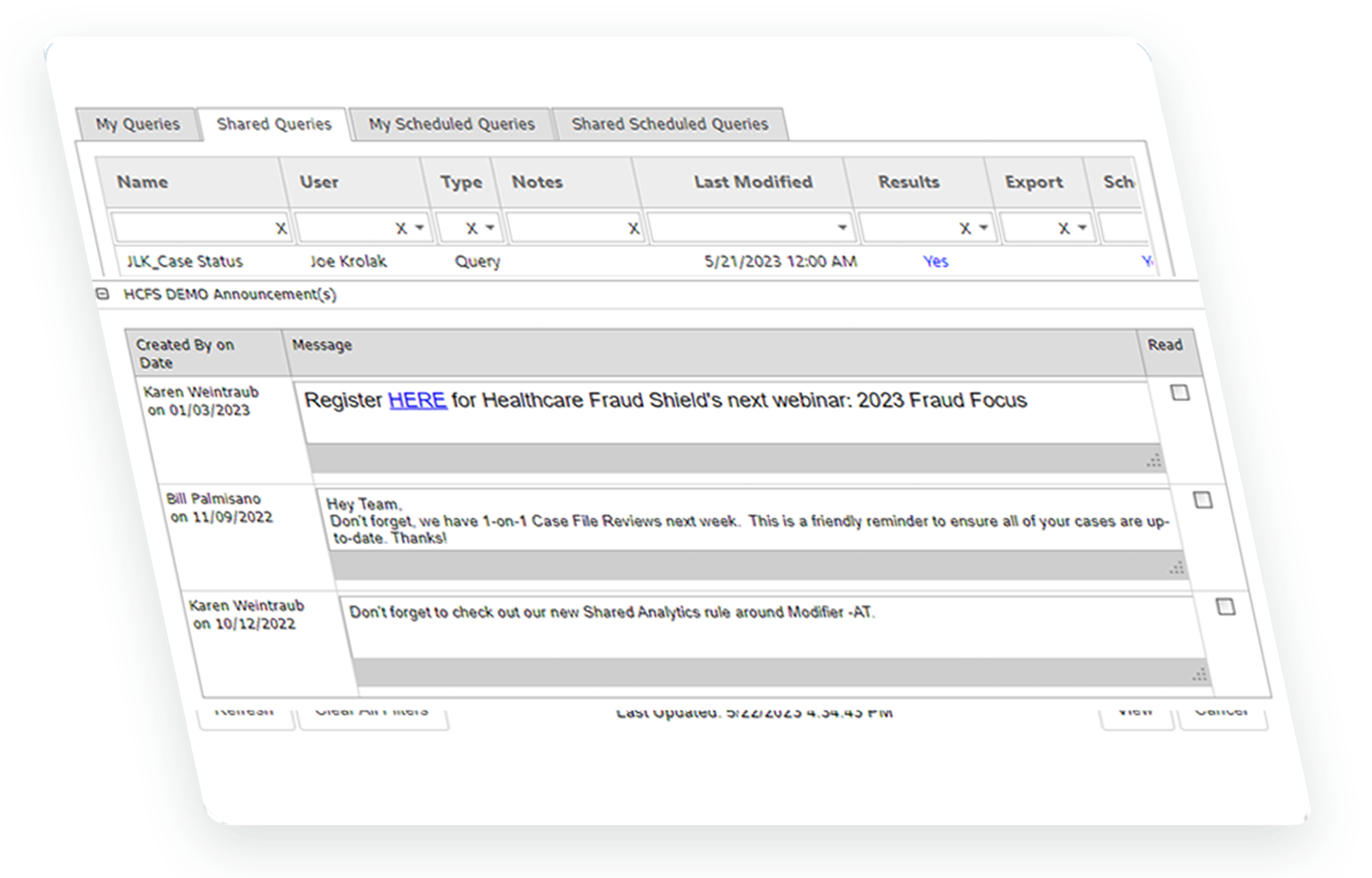
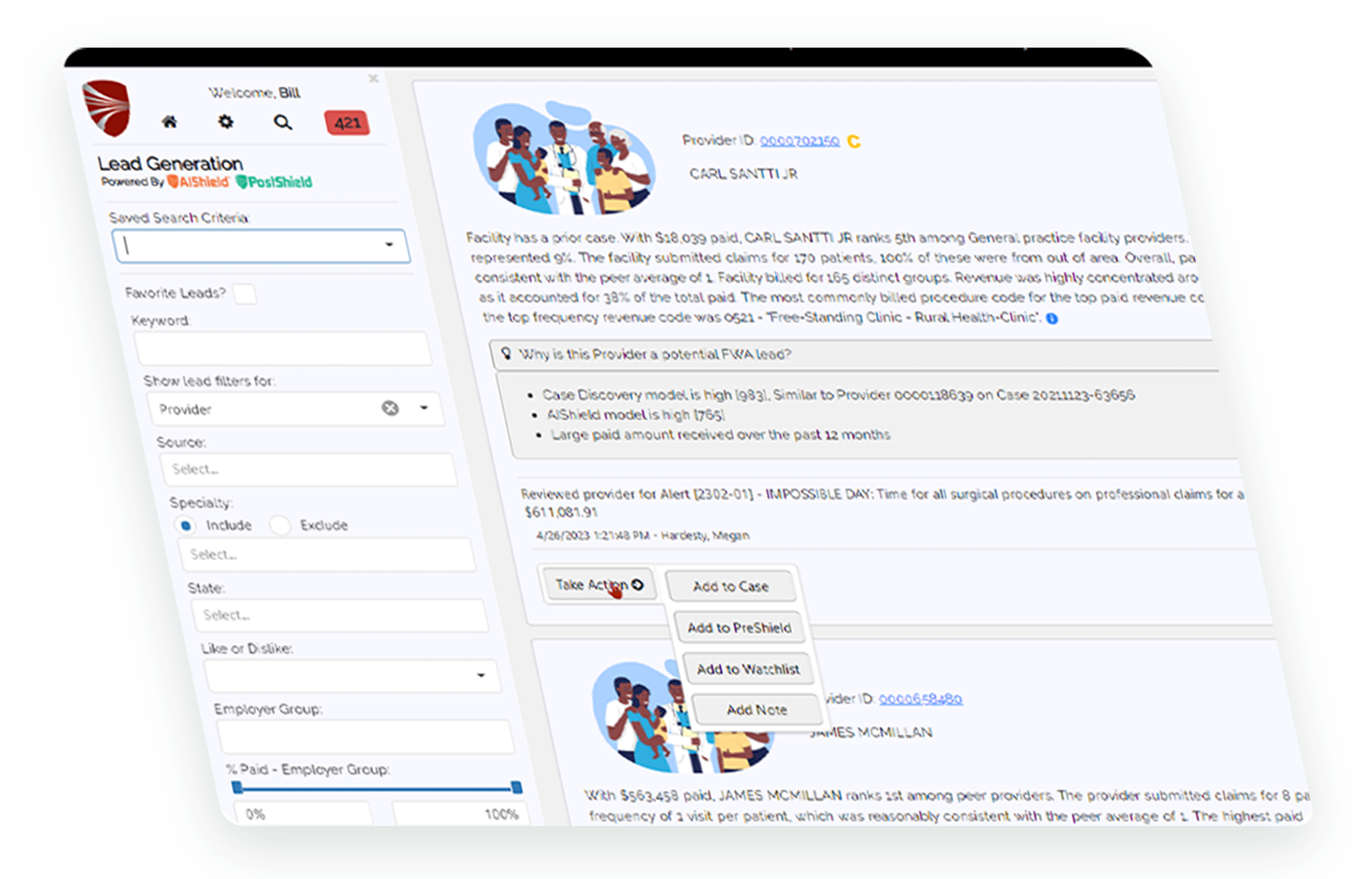
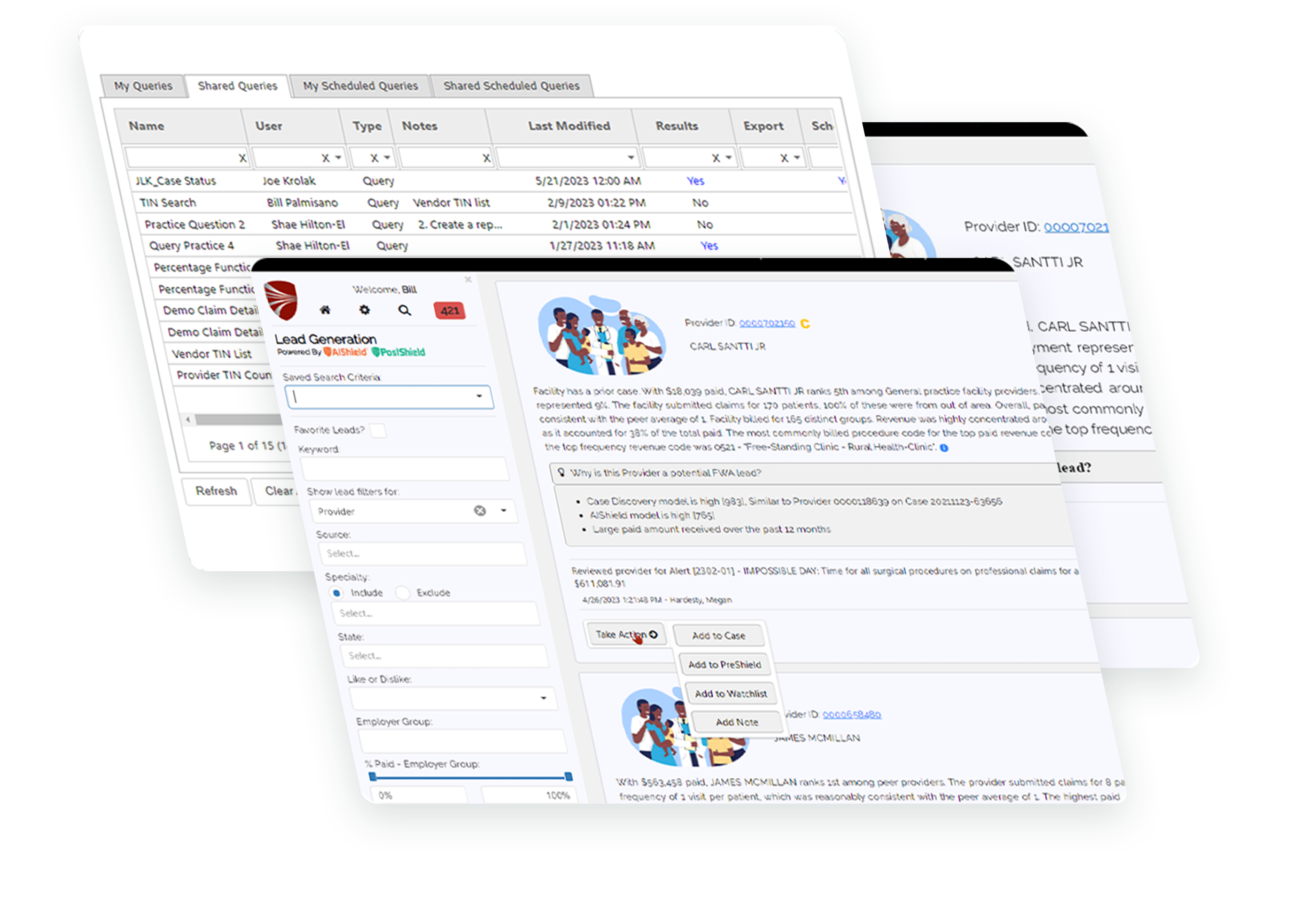
AIShield™ is a highly advanced artificial intelligence module that fully integrates with the HCFS Platform™ to detect and keep pace with the constantly evolving fraud, waste, and abuse schemes that are putting your payment integrity at risk.
Designed and validated using known healthcare fraud, waste and abuse cases, it has superior prediction capability and accuracy.
Product Features

Data visualization with highly intuitive UI to quickly isolate providers of interest.

Natural language generation to summarize the story of the behaviors of a provider.

Designed by subject matter experts with ease-of use top of mind.