Millions in Avoidable Losses Continue Across Federal Healthcare Programs
Is your integrity model board-ready?
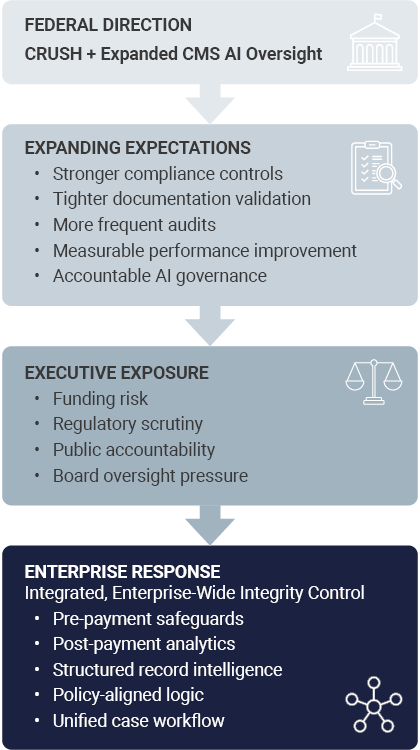
Oversight Expectations Are Evolving
Recent actions by the Centers for Medicare & Medicaid Services, including the Comprehensive Regulations to Uncover Suspicious Healthcare initiative and expanded artificial intelligence oversight, signal a measurable shift in how program integrity performance is evaluated.
Health plans and government programs are being asked to demonstrate not just the presence of controls, but measurable, defensible results.
Executive leadership teams must now answer a different question: Can we clearly prove that our integrity framework is working?
Federal Oversight Is Intensifying
Federal focus on payment integrity is sustained and structural.
Current signals include:
-
- Increased documentation validation requirements
- Heightened audit activity across high-risk service lines
- Expanded scrutiny of AI-driven payment oversight
- Greater transparency expectations around enforcement actions
Improper payments across Medicare and Medicaid programs continue to represent significant financial exposure. Oversight performance is now closely tied to funding confidence, public accountability, and governance visibility.
Program Integrity Maturity Comparison

From Analytics to Enterprise Control
Many organizations have invested in advanced analytics. Fewer have built enterprise-integrated program integrity infrastructure.
Analytics-driven models often include:
-
-
Rules-based pre-payment edits
-
Recovery-focused post-payment analytics
-
Operational dashboards
-
Limited AI decision traceability
-
Enterprise-integrated integrity programs align:
-
- Configurable, risk-based safeguards
- Integrated prevention and detection
- Structured documentation intelligence
- Unified workflow accountability
- Board-ready performance reporting
- Policy-aligned, auditable decision logic
Without integration across these functions, demonstrating measurable and defensible oversight becomes increasingly complex. Mature integrity programs connect oversight functions across the enterprise. This integrated model strengthens control consistency, improves transparency, and supports accountable AI governance.
Prevention
Pre-payment safeguards aligned with risk
Detection
Post-payment analytics integrated with prevention
Documentation Intelligence
Structured validation of medical records
Executive Visibility
Clear, board-level reporting of measurable performance
Supporting Measurable Oversight Performance
Healthcare Fraud Shield provides modular, AI-powered program integrity infrastructure designed to help health plans and government programs demonstrate defensible, policy-aligned oversight performance.
The HCFSPlatform integrates:
-
-
Pre-payment safeguards
-
Post-payment analytics
-
Structured documentation intelligence
-
Policy-aligned logic and decision governance
-
Unified case management workflow
-
Executive-level performance reporting
-
This enterprise-wide approach enables measurable improvement and sustained oversight performance.

Questions?
Email us at [email protected]
