Recent actions by the Centers for Medicare & Medicaid Services (CMS), including targeted spending reviews and the Comprehensive Regulations to Uncover Suspicious Healthcare initiative, known as CRUSH, reflect a measurable shift in federal oversight expectations.
CMS leadership has also signaled increased investment in artificial intelligence to strengthen fraud detection and payment oversight, reinforcing a broader move toward earlier risk identification and stronger contractor accountability.
Regulators are placing greater emphasis on demonstrable program integrity performance across high-risk service lines. For executive leadership teams, this shift carries implications for financial stability, compliance maturity, and governance oversight.
Oversight and Funding Stability Are Increasingly Connected
CMS has identified elevated and anomalous spending patterns in areas such as personal care services, home health, and durable medical equipment.
Program integrity performance is no longer viewed solely as an operational function. It is an essential component of financial stewardship.
Payer and Government Actions Signal Structural Controls
CMS implemented a temporary enrollment moratorium for certain durable medical equipment suppliers and reported substantial avoided fraudulent billing during that period. Plans and managed care organizations must be able to demonstrate consistent oversight across providers and members.
Organizations should consider strengthening:
- Eligibility controls for both providers and members
- Transparency related to revoked suppliers
- Fraud, Waste, Abuse, and Error (FWAE) detection and prevention
- Oversight abilities of technology partners supporting integrity efforts
These actions demonstrate an ongoing regulatory posture that prioritizes sustained safeguards rather than episodic enforcement.
CRUSH Points Toward Expanding Expectations
Through CRUSH, CMS is seeking additional FWAE prevention strategies that may shape future regulatory frameworks.
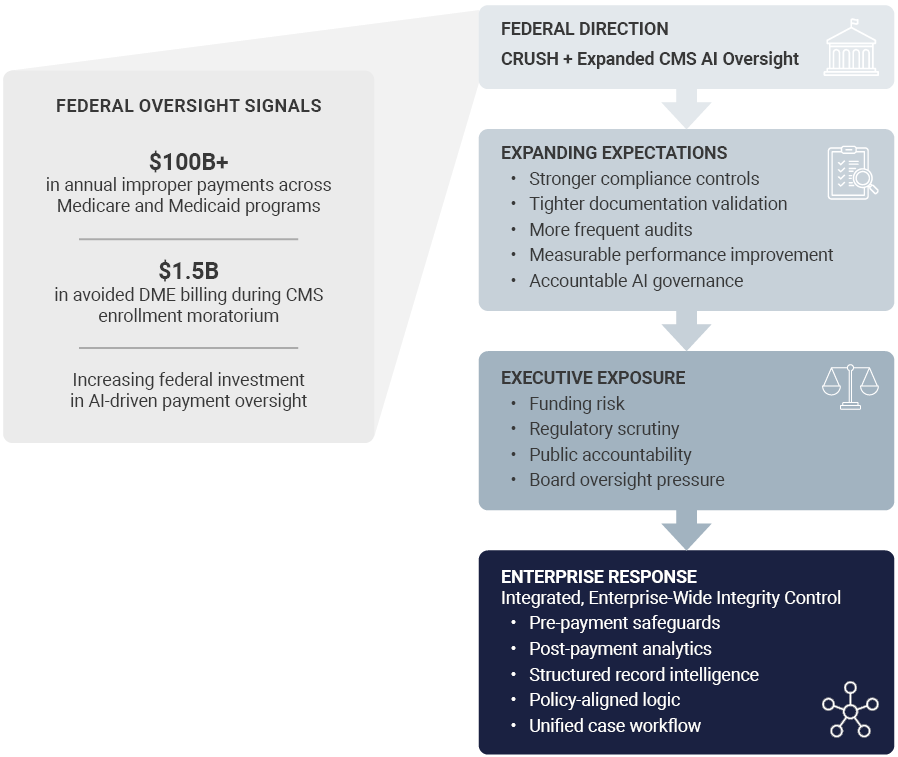
Organizations that rely on isolated analytics models or fragmented review processes may find it difficult to demonstrate enterprise-level control under these evolving expectations.
The Program Integrity Maturity Gap
Many healthcare organizations have invested in advanced data analytics, but fewer have built integrated program integrity infrastructure that connects prevention, detection, documentation validation, and executive reporting into a unified framework.
Program Integrity Maturity Comparison

Without integration across these functions, demonstrating measurable, defensible oversight becomes increasingly complex.
Aligning Infrastructure With Regulatory Direction
Healthcare Fraud Shield (HCFS) works with health plans and state programs to implement an enterprise-wide solution, with both a targeted and AI-powered program integrity infrastructure designed to meet evolving federal expectations.
The HCFSPlatform™ integrates:
- Pre-payment safeguards
- Post-payment analytics
- Structured medical record intelligence
- Policy-aligned logic
- Case tracking workflow
This unified approach enables organizations to strengthen controls, improve visibility, and support defensible program integrity performance.
Executive Takeaway
Federal oversight expectations are evolving. Transparency is increasing. Funding stability is increasingly connected to demonstrable program integrity performance.
Organizations that treat program integrity as integrated enterprise infrastructure will be better positioned to meet these expectations. Those operating with disconnected tools or reactive processes may face increasing pressure to demonstrate control.
The core question for executive leadership is straightforward:
Can your organization clearly and confidently demonstrate that its program integrity framework is delivering measurable, defensible results?

